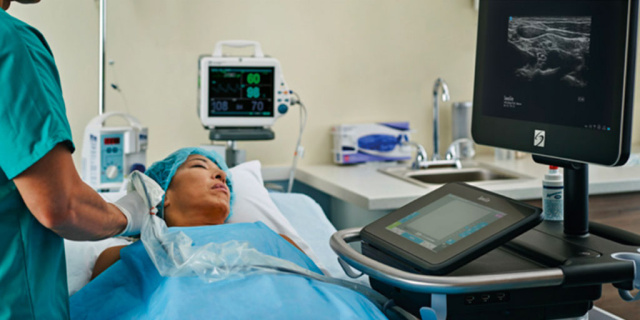
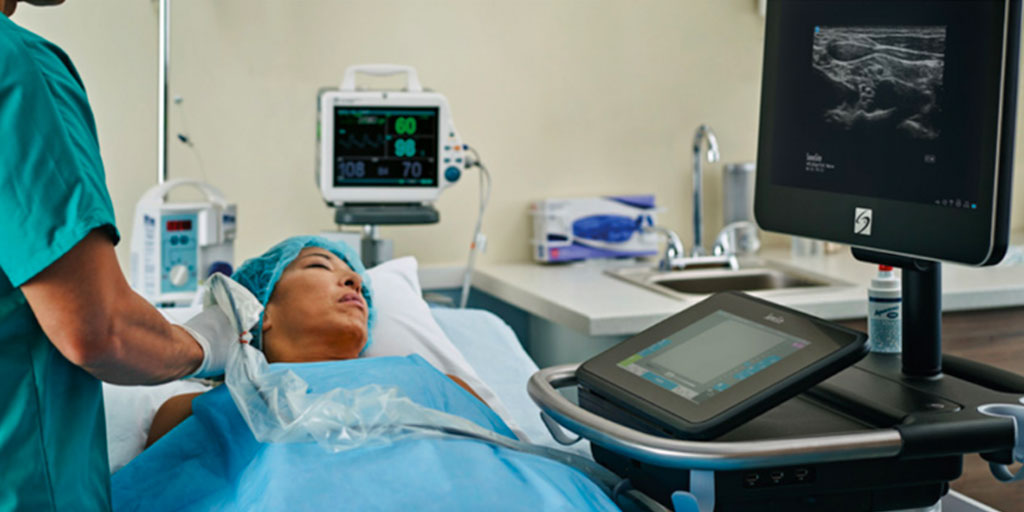
The use of opioids in the ICU and the post-operative period is common, with patients often receiving opioids even after simple surgeries. Though opioids are effective in providing fast pain relief, the side effects of respiratory depression, cough suppression, confusion, drowsiness, nausea, vomiting and potential addiction make the sole reliance on opioids risky.
ICU clinicians are formulating more effective strategies to manage patient pain while minimizing the risks. In an article published in ICU Management and Practice, Dr. Xavier Capdevila, Head of the Department of Anesthesia and Critical Care Medicine at Lapeyronie University Hospital, France, outlines the concept of multimodal analgesia as an alternative to administering solely opioids to patients.
The Multimodal Analgesia Approach
- Multimodal analgesia in the ICU includes the following strategies:
- Using non-opioid analgesics such as NSAIDs (anti-inflammatory drugs) in combination with (low dose) opioids whenever possible
- Prescribing the lowest effective dose of an opioid to limit the risk of addiction
- Using analgosedation, or using analgesia before administering sedatives
- Using light sedation rather than deep sedation whenever possible
- Combining regional anesthesia and epidural analgesia with analgosedation
Non-Opioid Drugs
Dr. Capdevila points out that in many cases the use of a non-opioid drug is a better choice for the patient. The combined use of these analgesics allows clinicians to administer lower total doses. These lower doses in turn reduce the number of side effects. As a result, multimodal analgesia can reduce postoperative pain (Jin and Chung 2001).
Analgesia before Sedation
Multimodal analgesia also reduces the need for total sedation. The practice of analgosedation in the ICU (using analgesia before sedation) is becoming increasingly common. One study demonstrated that patients who received more fentanyl and fewer benzodiazepines or more dexmedetomidine and less propofol required lower sedation (Faust et al. 2016).
A French study showed that the use of multimodal analgesia in mechanically ventilated critically ill patients decreases sedation and delirium while avoiding the need for opioids. Patients given multimodal analgesia were also more likely to have fewer organ failures compared to patients who received opioids alone (Payen et al. 2013). Dexmedetomidine, an alpha 2 antagonist and a potent anxiolytic, is another drug that ICU clinicians should consider within the multimodal analgesia approach. Dexmedetomidine has shown to limit the duration of mechanical ventilation compared to Midazolam (Jakob et al. 2012). However, Dr. Capdevila points out that more studies are needed to compare this drug’s benefits versus its adverse side effects.
Regional Anesthesia and Epidural Analgesia
A study published in Anesthesia and Analgesia compared patients with a paravertebral blockade with rib fractures who received only sedation and opioids to similar patients who also received regional anesthesia. The patients who received regional analgesia experienced an optimized rehabilitation with a decreased use of opioids. The mixed use of sedative agents with opiates coupled with regional anesthesia helped improve patient rehabilitation in the postoperative period (Malekpour et al. 2017).
The addition of epidural analgesia to general anesthesia was also associated with long-term survival. A study published in JAMA Surgery analyzed patients who received abdominal aortic aneurysm repair. Patients who received epidural analgesia exhibited fewer complications than patients who received only analgosedation (Bardia et al. 2016). Clinical evidence shows that epidural analgesia can decrease mortality, complications, and morbidity after surgery. Epidural analgesia also limits the need for opiates, thereby decreasing opioid-related complications (Pöpping et al. 2014).
Through the proper application of multimodal analgesia, ICU clinicians can effectively manage patient pain while reducing the need for opioids and heavy sedation. Dr. Capdevila concludes multimodal analgesia optimizes pain management and decreases organ dysfunction while demonstrating a positive impact on the long-term mortality in patients after major surgeries.
References
Bardia A, Sood A, Mahmood F, Orhurhu V, Mueller A, Montealegre-Gallegos M, Shnider MR, Ultee KH, Schermerhorn ML, Matyal R et al. (2016). Combined Epidural-General Anesthesia vs. General Anesthesia Alone for Elective Abdominal Aortic Aneurysm Repair: JAMA Surgery, 151(12):1116-1123.
Capdevila, X. (2019, Spring). Pain management through multimodal analgesia in the ICU: ICU Management and Practice, Volume 19, Issue 1. Retrieved from https://healthmanagement.org/uploads/article_attachment/icu-v19-i1-xavier-capdevila-pain-management-through-multimodal-analgesia-in-the-icu.pdf (VI-VIII).
Faust AC, Rajan P, Sheperd LA, Alvarez CA, McCorstin P, Doebele RL et al. (2016). Impact of an Analgesia-Based Sedation Protocol on Mechanically Ventilated Patients in a Medical Intensive Care Unit: Anesthesia Analgesia, 123(4):903-9.
Jakob et al. (2012). Dexmedetomidine vs. midazolam or propofol for sedation during prolonged mechanical ventilation: two randomized controlled trials: JAMA, 307(11):1151-60.
Jin F and Chung F (2001). Multimodal Analgesia for Postoperative Pain Control: Journal of Clinical Anesthesia, 13:524- 539.
Malekpour M, Hashmi A, Dove J, Torres D, Wild J et al. (2017). Analgesic choice in management of rib fractures: paravertebral block or epidural analgesia?: Anesthesia and Analgesia, 124:1906-11.
Payen JF, Genty C, Mimoz O, Mantz J, Bosson JL, Chanques G et al. (2013). Prescribing non-opioids in mechanically ventilated critically ill patients: Journal of Critical Care, 28(4):534.e7-12.
Pöpping DM, Elia N, Van Aken HK, Marret E, Schug SA, Kranke P, Wenk M, Tramèr MR et al. (2014). Impact of epidural analgesia on mortality and morbidity after surgery: systematic review and meta-analysis of randomized controlled trials: Annals of Surgery, 259(6):1056-67.

