Beginning on January 1, 2020, the Center for Medicare and Medicaid Services (CMS) launched a new appropriate use criteria (AUC) program for advanced diagnostic imaging services provided to Medicare beneficiaries. The purpose of the new program, enacted as part of the Protecting Access to Medicare Act (PAMA) signed into law in 2014, is to address the overutilization of MRI, CT, nuclear medicine, and PET scans.
Shoulder pain, including suspected rotator cuff injury, is one of eight initial clinical areas CMS had identified to review for overutilization and ordering patterns that are inconsistent with evidence-based AUC developed or endorsed by national professional medical specialty societies or other provider-led entities. The other priority clinical areas included in the initial phase of the AUC program are coronary artery disease, suspected pulmonary embolism, headache, hip pain, low back pain, cancer of the lung, and cervical or neck pain.
An Educational and Operations Testing Period of the new AUC program began on January 1, 2020 and will last through December 31, 2020. During this period, ordering clinicians are required to consult a qualified Clinical Decision Support Mechanism (CDSM) prior to ordering a Medicare Part B CT or MRI to assist them in making the most appropriate treatment decision for a patient’s shoulder pain. The ordering clinician must also provide this information to the professional providing the imaging service, who will in turn report a HCPCS modifier on their claims with the appropriate CT or MRI CPT code. CMS will not deny a claim that incorrectly reports AUC information during this period of the program. Starting in 2021, however, advanced diagnostic imaging service claims without the appropriate AUC coding information will be rejected. This requirement does not apply to the ordering of a diagnostic ultrasound service used to make a treatment decision for a patient’s shoulder pain.
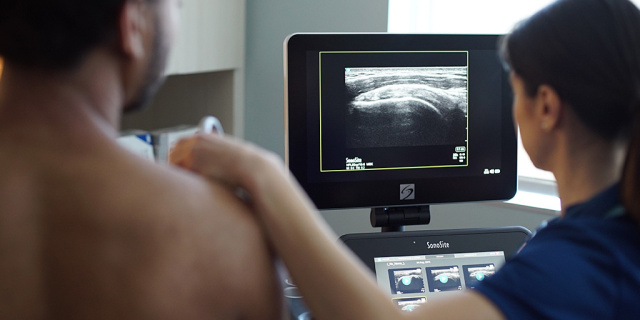
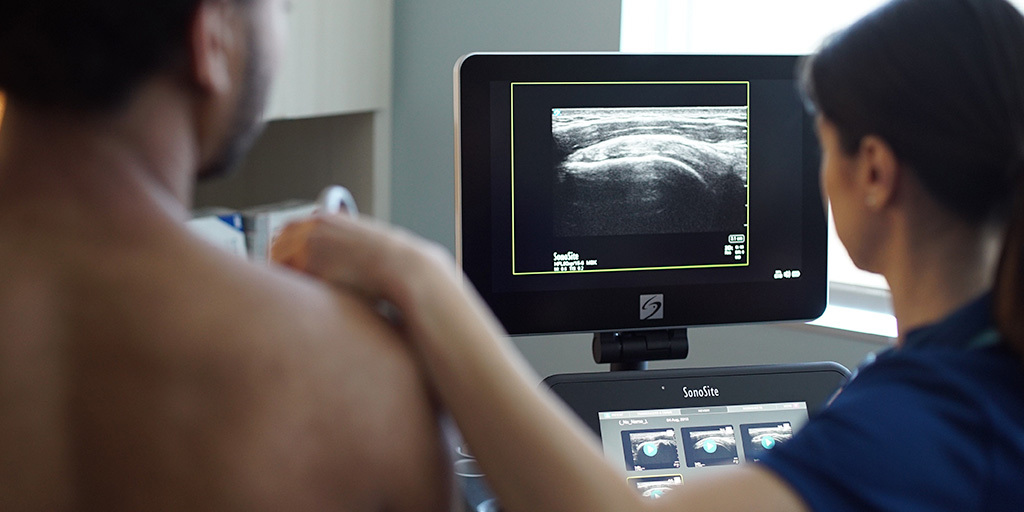
The new AUC program responds to concerns about inappropriate use of advanced diagnostic imaging services and the escalating costs to the healthcare system resulting from overuse of these services. Healthcare providers in general have used more expensive imaging modalities such as CT and MRI instead of ultrasound as the first diagnostic test for many musculoskeletal injuries, including shoulder injuries. However, ultrasound is a lower cost alternative with clear advantages. For example, ultrasound can easily scan both shoulders, allowing a comparison of healthy and damaged joints, which can be very useful in diagnosing shoulder and other musculoskeletal injuries.
Looking back at cost data regarding MSK imaging in 2009 alone, CT and MRI accounted for 95% of Medicare allowed charges for all extremity imaging. Only 5% was for ultrasound, which is cost-effective and avoids the inherent risk of radiation exposure. An article by Parker, et al. published in 2008 indicates that the substitution of musculoskeletal ultrasound for musculoskeletal MRI, when appropriate, would lead to savings to Medicare of more than $6.9 billion in the period from 2006 to 2020.
Ultrasound has become more popular overtime due to its accuracy, efficiency, portability, and lower cost. The new federal AUC program further underscores the value of ultrasound as a low-cost, effective alternative for use in diagnosing shoulder pain and other musculoskeletal conditions.
1Parker, et al. Musculoskeletal imaging: Medicare use, costs, and potential for cost substitution. Journal of American College of Radiology. 2008: 182:188.

