Iatrogenic Pneumothorax Complications: Zero
The prestigious Memorial Hermann Healthcare System achieved zero iatrogenic pneumothorax complications for one year. Learn how they achieved this feat in several of its hospitals and eight of its community hospital emergency departments.
Improving Quality of Care and Patient Safety While Saving Money
Multiple studies have demonstrated that ultrasound guidance improves the success rate and safety of invasive procedures including central venous lines, paracentesis and thoracentesis. Avoiding complications is not only is good for patient care, it reduces the overall cost of care for hospitals. A recent study conducted by United BioSource Corporation (UBC) demonstrated this cost reduction. Two recent studies, presented at the 2011 National Patient Safety Foundation (NPSF) Annual Meeting, found significant economic savings when ultrasound guidance was used as part of the care pathway. The largest studies of their type, they examined both paracentesis and thoracentesis and found fewer complications in the ultrasound guided group as well as substantial cost savings. As an example, a single iatrogenic pneumothorax increased hospital costs by more than $2,700 and a single bleeding complication during a paracentesis increased hospital costs over $20,000. Furthermore, both groups with complications had significantly longer hospital length of stays. Read more below on the economic and safety benefits of patients receiving ultrasound guidance for their thoracentesis or paracentesis.
Evidence Shows Ultrasound Guidance Reduces Paracentesis and Thoracentesis
Real-time ultrasound guidance significantly improves first-pass procedural success and improves patient safety for a number of needle-based procedures, including central lines, thoracentesis and paracentesis.
Complications from Paracentesis: Hemorrhage, Hematoma, Hemoperitoneum
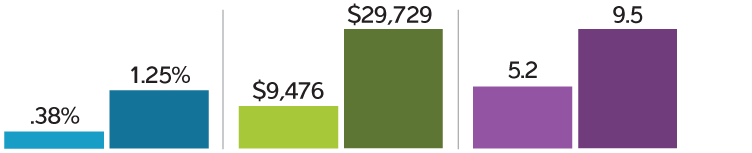
Risk of Hemorrhage, Hematoma, Hemoperitoneum Occurence with and without Ultrasound Guidance for Paracentesis
Ultrasound Guidance No Ultrasound Guidance
Hospitalization Costs with and without Complications from Iatrogenic Hemorrhage, Hematoma, Hemoperitoneum
Without Complications With Complications
Length of Hospital Stay (days) with and without Complications from Hemorrhage, Hematoma, Hemoperitoneum
Without Complications With Complications
For the 69,859 patients who underwent a paracentesis, suffering a bleeding complication boosted hospital costs to nearly $30,000, about triple the cost for patients without a complication ($9,476) and length of hospital stay almost doubled, from a mean of 5.2 days for a patient without a bleeding complication to a mean of 9.5 days for a patient with one. Read the paracentesis abstract
Complications from Thoracentesis: Pneumothorax
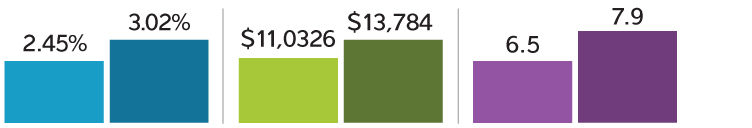
Risk of Iatrogenic Pneumothorax Occurence with and without Ultrasound Guidance
Ultrasound Guidance No Ultrasound Guidance
Hospitalization Costs with and without Complications from Iatrogenic Pneumothorax
Without Complications With Complications
Length of Hospital Stay (days) with and without Complications from Iatrogenic Pneumothorax
Without Complications With Complications
For the 61,261 patients included in the analysis who underwent a thoracentesis, ultrasound guidance reduced the incidence of a pneumothorax by 19%. This complication increased a patient's hospital cost to $13,784, compared to $11,032 for a patient who didn't suffer a pneumothorax. In addition, the mean length of hospital stay was 7.9 days for a patient with a pneumothorax, versus 6.5 days for a patient without it. Read the thoracentesis abstract
The studies, "Clinical and Economic Advantage of Ultrasound Guidance Among Patients Undergoing Paracentesis" and "Clinical and Economic Advantage of Ultrasound Guidance Among Patients Undergoing Thoracentesis" were completed for Sonosite by the United BioSource Corporation (UBC), a global scientific and medical affairs organization. Researchers from the UBC Center for Epidemiology and Database Analytics used the national Premier Perspective® automated hospitalization claims database to access thousands of patients' records in over 600 hospitals from across the country.
The Recommendations are Clear
Based on this robust evidence, multiple government organizations and societies advocate ultrasound guidance:
- AHRQ – Agency for Healthcare Research and Quality
- NICE – National Institute for Health and Clinical Excellence
- CDC – Centers for Disease Control and Prevention
- American College of Surgeons
- American College of Emergency Physicians
- American College of Chest Physicians
- American Board of Internal Medicine
- Association for Vascular Access
Let Us Help You Lessen Line Placement Complications at Your Hospital
Sonosite is committed to quality care and partners with hospitals to achieve that goal. To facilitate the process, Sonosite has created the Central Line Management Program. This evidence-based program includes AHRQ, CDC and IHI recommendations and addresses both mechanical and infective complications of central venous catheters, allowing you to decrease:
A) Accidental punctures causing pneumothorax, hemothorax, or carotid injury
B) Central line associated bloodstream infections (CLABSI)

