Dr. Philippe Mahiou practises anaesthesia in the Grenoble area of France, splitting his time between a private clinic and working as a helicopter doctor attending mountaineering accidents. As part of his work, Dr. Mahiou routinely uses ultrasound, and understands the importance of the technology for both guiding anaesthesia in the operating room and assessing patients in the field.
Around 80% of my work is at the Clinic des Cèdres, a private clinic near Grenoble, where approximately 7,000 to 8,000 trauma and orthopaedic procedures are performed every year. I frequently use ultrasound to guide injections for regional anaesthesia. The main advantage is that you can visualise the nerve very precisely, and it’s not necessary to use neuro-stimulation to look for the nerves instead.
Our Sonosite systems offer excellent image quality; you can even visualise nerves in the feet, which are very small and often hard to see. It is also easy to move the systems around and adjust their height, which is perfect for point-of-care applications. Additionally, we can save images and export them which is great for teaching, as are the regional anaesthesia educational ultrasound training videos on our X-Porte systems.
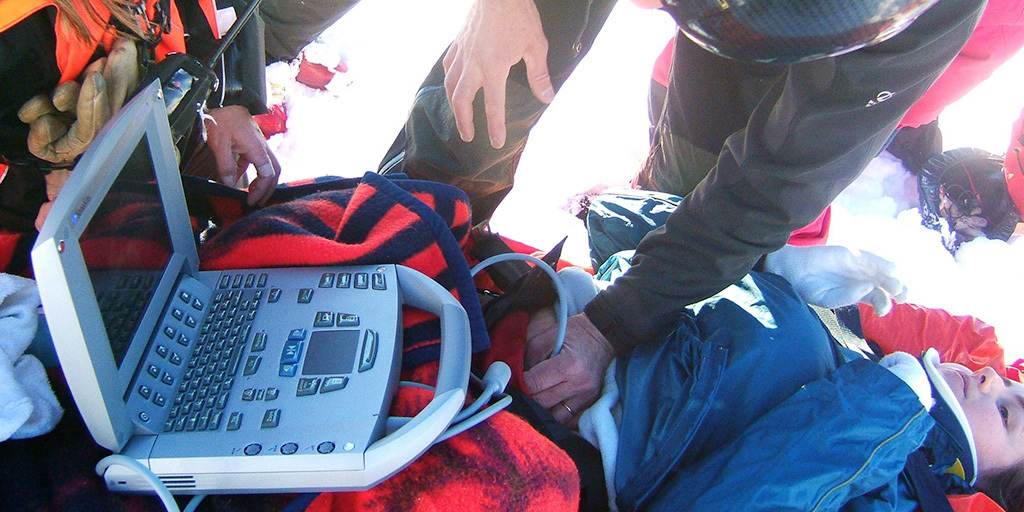
The remaining 20% of my work is as a mountain rescue doctor for the Grenoble University Hospital. People that have mountaineering accidents often suffer from all kinds of thoracic, cerebral, abdominal, spinal, and pelvic injuries, and so it’s vital for us to reach and treat the patient as quickly as possible. We’re the second largest mountain rescue base in France after Chamonix, and receive about 1,000 calls per year.
The team is made up of five individuals; a pilot, a mechanic, two rescuers, a doctor such as myself and, in avalanche cases, we often also use rescue dogs. We carry the same kit as an emergency department—all the equipment necessary to resuscitate in the field—packed in to two bags. The first bag carries all of the equipment to reduce and try to stop heavy bleeding or treat patients suffering from cardiac arrest, as well as our portable ultrasound system, while the second bag contains supplementary equipment for resuscitation.
We use ultrasound as part of the clinical examination of each patient to diagnose any problems, assist with pain management, and monitor them on route to hospital. When we arrive at a patient, we start by checking the pulse, blood pressure, and respiratory rate before performing an ultrasound scan. We begin with a FAST examination—to check whether there are any transabdominal effusions—then we use ultrasound to guide regional anaesthesia for pain management, including femoral, interscalene, infraclavicular, medial, radial, and ulnar blocks as required.
We often also conduct pulmonary, cardiac, and transcranial Doppler ultrasounds to help us decide which hospital is best to send the patient to, depending on the severity of the trauma. A lot of our patients suffer from cranial injuries, and identifying these means we can send patients straight to the neurosurgery department on arrival at the hospital for more immediate emergency treatment. Another benefit of ultrasound is that you can use it to monitor a patient if their health is deteriorating. For instance, we regularly repeat FAST examinations and discover transabdominal effusions that hadn’t had time to form before we conducted the initial scan. Overall, ultrasound is a really valuable and versatile tool both in the clinic and out in the field. It has improved the quality of patient care, and I don’t know what I’d do without it.
More about Sonosite Systems for Emergency Services
In Case of Emergency, Use POCUS

