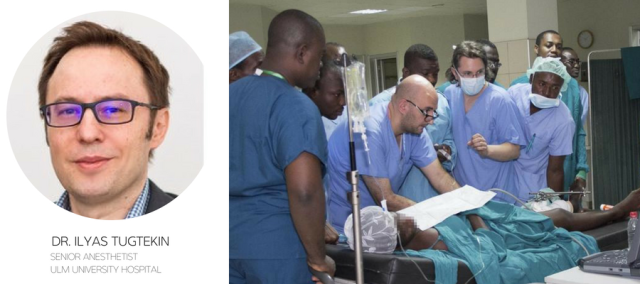
Dr. Ilyas Tugtekin, a consultant anesthetist from Ulm University Medical Center in Baden-Württemberg, Germany, travels to Kumasi, Ghana to help establish an ultrasound training center for doctors all over West Africa.
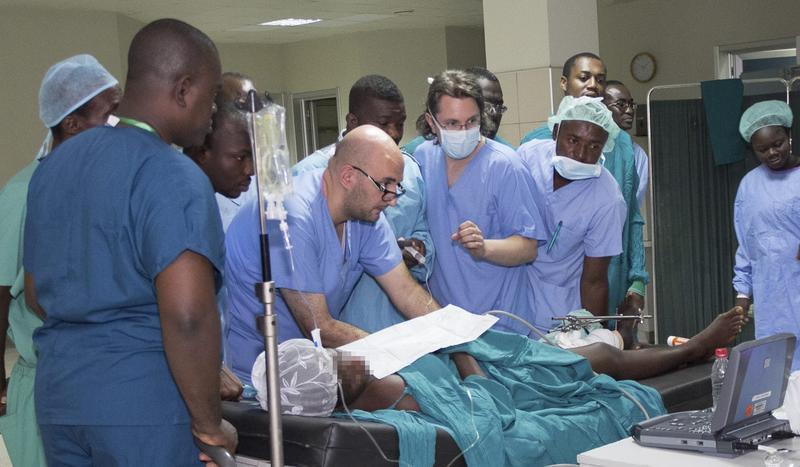
Funded by the Else Kröner-Fresenius Foundation – a non-profit organization dedicated to supporting medical research and related humanitarian projects – a team of five specialists spent a week at Ghana’s second largest hospital, the 1,000-bed Komfo Anokye Teaching Hospital (KATH) in Kumasi, teaching ultrasound-guided techniques, including POCUS-guided regional nerve blocks, to clinicians from across the region. In this dispatch Dr. Ilyas Tugtekin discusses the experience and program.
Regional nerve blocks are ideally suited to a range of procedures, from trauma surgery to orthopedics. A regional block can be used as a standalone procedure for ambulatory surgery, or in combination with a general anesthetic to provide post-operative pain relief. Ultrasound guidance is vital to perform efficient and effective regional anesthesia, and I have been using this technique in my own practice for trauma and orthopedics, particularly hand surgery, for over 12 years.
Around 12 years ago, two doctors from Kumasi came to Ulm to undertake their specialist training in general anesthesia, which included using point-of-care (POC) ultrasound to guide vascular access and regional blocks. Not surprisingly, they saw huge potential for using ultrasound guidance in their hospitals back in Ghana. Kumasi itself is a large city with a population of more than two million and there are comparatively high numbers of trauma cases – the result of inferior road systems and working conditions – with patients frequently driven to hospital by relatives or by taxi.
Ultrasound-guided regional anesthesia and vascular access would be hugely beneficial for doctors in a developing country, allowing more rapid, safer procedures with faster recovery times and fewer complications. Soon after their return to Ghana, I visited KATH and held a small workshop as a starting point. Many of the doctors in the region are highly motivated, but lack the resources to implement this technology and so, together with our colleagues in Kumasi, we were keen to develop a local teaching program and center for ultrasound-guided procedures. We were able to gain the support of EKFS, which generously funded both the purchase of two robust point-of-care ultrasound systems for KATH and a training course for local doctors. A group of five specialist trainers – myself, Dr. Wolfgang Stahl and Dr. Alexander Dinse from Ulm, Dr. Oliver Vicent from the University of Dresden, and Dr. Gernot Gorsewski from the Landeskrankenhaus Feldkirch in Austria – spent a week running this course in Kumasi.
It was very well attended. There were over 30 delegates, not just from Kumasi, but also from the Ghanaian capital of Accra and further afield, including doctors from the Lebanon, Nigeria and Cameroon. We covered a number of basic ultrasound-guided procedures during the course, but focused on regional nerve blocks and venous access, as these are the most widely applicable techniques. The course was set up to be predominantly hands-on training, not just lectures, so it was very interactive. The delegates were able to spend time getting familiar with using the instruments in the workshops – finding the nerves on live models and performing punctures on phantoms themselves – and then we did some closely supervised nerve blocks and vascular access with them in the hospital at the end of the course.
The ultrasound techniques they learned during the course will have a number of applications throughout the hospital. For example, there was one doctor on the course very interested in hand surgery, and regional anesthesia will allow many of his patients to go home almost straight after the procedure, requiring less post-operative care. There were also several emergency medicine physicians on the course and, for them, ultrasound-guided vascular access is extremely useful; it’s a lot safer, quicker, and more effective, which is a huge benefit in a very busy department with too few doctors.
Without access to suitable POC ultrasound systems, these newly acquired skills would be useless, so we were very pleased to be able to leave the ultrasound systems we had used during the course at KATH. The hospital needed robust and highly portable instruments that it could move around the hospital’s large theatre suite and use in the emergency department. This would improve the efficiency of many procedures and ultimately allow the team there to treat more patients. Following the success of this course, we are already hoping to return next year. Since my first visit in 2008, the hospital has already made vast improvements, most notably in the emergency department where they now use POC ultrasound to perform FAST and lung scans looking for pneumothorax; it would be nice to be able to return and help them develop more procedures using diagnostic ultrasound.
Ghana is quite lucky to have one of the best medical school systems in the region, and KATH currently has around 200 medical students beginning their training; my colleagues and I look forward to introducing the next generation of doctors to the benefits of this technology.